Arthritis in the hip joints is a common issue for many of our dogs as they age and particularly common in some specific breeds such as the Labrador Retriever, Great Dane, Rottweiler, German Shepherd Dog, St. Bernard and Bulldog. However, joint issues can affect any size dog and any breed.
One excellent tool for assessing for the risk of hip dysplasia is PennHIP imaging. Images can be taken at any age, including puppies as young as 4 months of age. Early evaluation can allow early intervention at a time when joints are still developing and before the onset of arthritis. Studies have shown that the degree of joint laxity (how loose the joint is) does not change significantly over time, and additional studies confirm that the same dog evaluated by different PennHIP veterinarians will have very similar scores. This ability to reproduce the results consistently is key and most importantly, PennHIP imaging has been documented to be the best predictor of future development of osteoarthritis.
We are recognizing Gabi as our Pet of the Month for October.
She is a lovely 7-year-old Border Collie/Poodle mix who didn’t show any signs of joint issues until there was quite a bit of change present. Surprisingly, this is often the case with many dogs. The dogs don’t know that their joints should feel a particular way, and many hide their symptoms in the early stages. Depending on their size and lifestyle owners may easily miss a subtle limp, a shift in gait, or a reluctance to play fetch as long as usual. And for active dogs, it is common to think limping or soreness is just a consequence of rough and tumble play or over activity . Gabi, who is a medium sized dog, was quite active with her owner, regularly going to the dog park and on hikes around the area, yet she never complained.
In 2019 the doctors at Hawthorne Hills Veterinary Hospital took radiographs of Gabi’s abdomen as part of an evaluation for intestinal issues. The hip joints were visible on the edge of the film and the radiologist made mention that Gabi had hip dysplasia. This was an ‘incidental finding’ as Gabi wasn’t having any symptoms of discomfort, changes in mobility or activity but we discussed with her owner what symptoms to watch for, steps to take to reduce stress on the hips and how to keep Gabi comfortable.
We discussed taking PennHIP radiographs, and for a variety of reasons they were postponed. Then COVID-19 happened. It wasn’t until November 2020 that we were able to schedule Gabi’s radiographs. At the time, Gabi’s physical exam was normal without any reduction in her range of motion and no specific hip pain. The owner had noticed Gabi would occasionally stop while running and look back at her left hip. This was a such a minor change that he says he only noticed because we had explained the symptoms to watch for; otherwise, he would have ignored it.
While we knew Gabi had hip changes, we still opted to perform the PennHIP imaging. The question is, why take the PennHIP images if you know the hips are already bad? First of all, documenting the degree of laxity and change can be helpful, the images help us to assess the amount of arthritic change over time and having Gabi entered into the PennHIP database helps every other dog.
In Gabi’s case, we elected to combine her sedated hip imaging with a planned dental procedure which required anesthesia anyway. Pursuing the best diagnostic and treatment plan was the goal of Gabi’s owner. The PennHIP report came back as ‘we are unable to effectively evaluate the degree of laxity because of ‘Severe Osteoarthritis’ already present in both hips. The progressive remodeling of the hip joint prevents an accurate measurement of the laxity’. We knew this would be the likely findings, and even though we didn’t get an actual DI value (distraction Index), by taking the images we can visually see how much laxity is present in Gabi’s joints and that is important going forward.
While Gabi’s hip disease was considered severe, her initial symptoms were mild. She did subsequently develop some episodes of lameness despite starting on therapy so Gabi and her owner were referred to Sound Veterinary Rehabilitation Center in Shoreline, WA for a long-term treatment plan focused at helping to slow the progression of her arthritis and to help her live more comfortably. For others contemplating a rehab consultation, are Sound Rehab’s stated goals of therapy.
-
- strengthen core muscles & overall body
- encourage movement without aggravating the arthritis
- maintain spinal flexibility
- maintain Range of Motion in all joints
- work to correct and prevent compensatory changes
- manage pain & inflammation
- weight management is also a key component; obtain and maintain a lean body mass
Fortunately for Gabi, she has responded well to therapy and has graduated to ‘at-home’ care. Her owner learned a number of techniques that he can continue at home to help maintain Gabi’s mobility and comfort. She is currently is well controlled with no appreciable symptoms of pain or discomfort and she is able to keep her active lifestyle.
WHY PENNHIP versus OFA IMAGING?
Knowing your dog’s risk for developing arthritis in the hips can help you make appropriate decisions that reduce the progression of changes and help your dog lead a more comfortable and pain free life. Selecting the best diagnostic tool is important.
PennHIP imaging requires the veterinarian to obtain specific certification to ensure consistent images, the evaluation utilizes an objective method to assess laxity in the hip joint, imaging must be done under sedation or anesthesia (which is the kindest thing for the dog who has arthritis), and the images must all be submitted to the national database. This aids in research and ensures that breeders and pet owners alike have full information. Every dog owner gets real data about how many individuals of a specific breed have hip dysplasia.
In situations where you know or suspect the dog has hip changes, some people ask, why not just do OFA imaging instead? OFA imaging is only one ‘hip extended’ view, the assessment is based on the dog’s conformation which is a subjective evaluation, and OFA imaging does not have the same evidence-based predictability for the risk of hip dysplasia in the future. Finally, and most importantly, OFA does not require every dog who is imaged to be entered into a national database. This alone skews the information available to breeders and prospective pet owners and renders the information less useful.
WHAT DO TREATMENT PLANS ENTAIL?
Generally plans will be tailored to the needs of the individual dog and the degree of arthritis they have. Here are common aspects of treatment.
- Therapeutic foods such as Hill’s j/d food, Purina JM, and Royal Canin Mobility
- Medications: NSAIDs – non-steroidal anti-inflammatory drugs, Adequan injections
- Omega 3 Fatty Acids – ask your veterinarian for the best products that have been evaluated for pets
- Joint supplements – not all are created equally – consult your veterinarian as to which ones have research and documented efficacy
- Assisi Loop (PEMF – pulsed electro-magnetic field therapy) – FDA approved device to help reduce inflammation in affected areas of the body
- Massage and specific exercises to strengthen muscles and to help maintain joint flexibility and movement
- Underwater treadmill sessions to build strength without stress on the joints
Here’s a link to another blog article we wrote on Hip Dysplasia. Do you know if your dog is at risk for hip dysplasia?
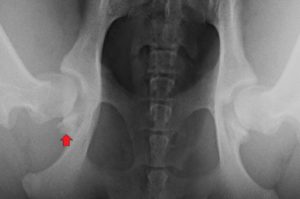
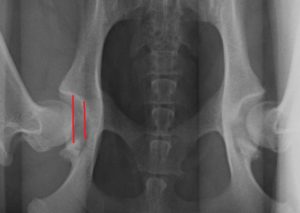
The first 3 images below are those of Gabi. The femoral heads are misshaped, there is evidence of boney change around the socket and the femoral heads do not fit smoothly and completely into the acetabulum. The second set of 3 images, are those of a dog with tight hips; the joint is well formed, the surfaces are smooth and there is almost no laxity as evident on the distraction view.
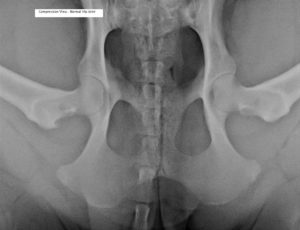
Normal hip joint – PennHIP Compression View. The ball of the femur is well seated in the socket and smooth with the acetabulum.
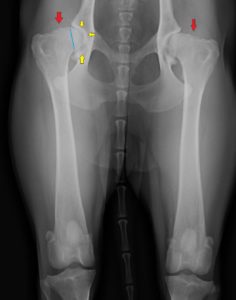
The red arrows point to arthritic change; the yellow arrows outline arthritis in the joint, and the blue line shows how little of the femoral bone is seated in the hip socket. This is the ‘Hip Extended’ view.
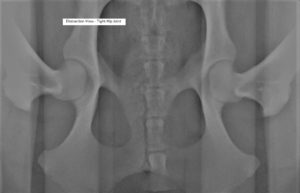
Normal Hip – PennHIP Distraction View. There is very little movement of the femur out of the socket as these hip joints are quite tight.
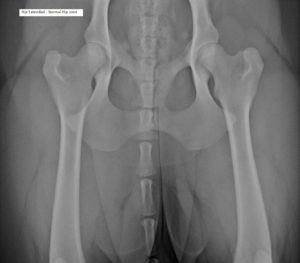
This Hip Extended View shows the femoral heads seated deeply into the sockets. These are normal hip joints.